Your Health Benefits
Ver en español | 查看中文 | 한국어로 보기 | Посмотреть на русском | Xem bằng tiếng việt | Переглянути укр | عربى | មើលជាភាសាខ្មែរ | Soomaali | ਪੰਜਾਬੀ
Your Care Begins with Healthcare Coverage
You have access to affordable, high-quality healthcare coverage, designed for caregivers. See below for links to detailed information about your health plan. Learn more about how to get covered.
Your Health Benefits
For more information about your specific plan or to access your Health Benefits Guide, select your health plan below.
KPWA HMO = Kaiser Permanente Washington HMO, KPNW HMO = Kaiser Permanente Northwest HMO, KPWA POS = Kaiser Permanente of Washington POS
What plan do I have?
Your specific health plan is automatically assigned based on your ZIP code. If you are not sure which plan you have, use the map below to find out:
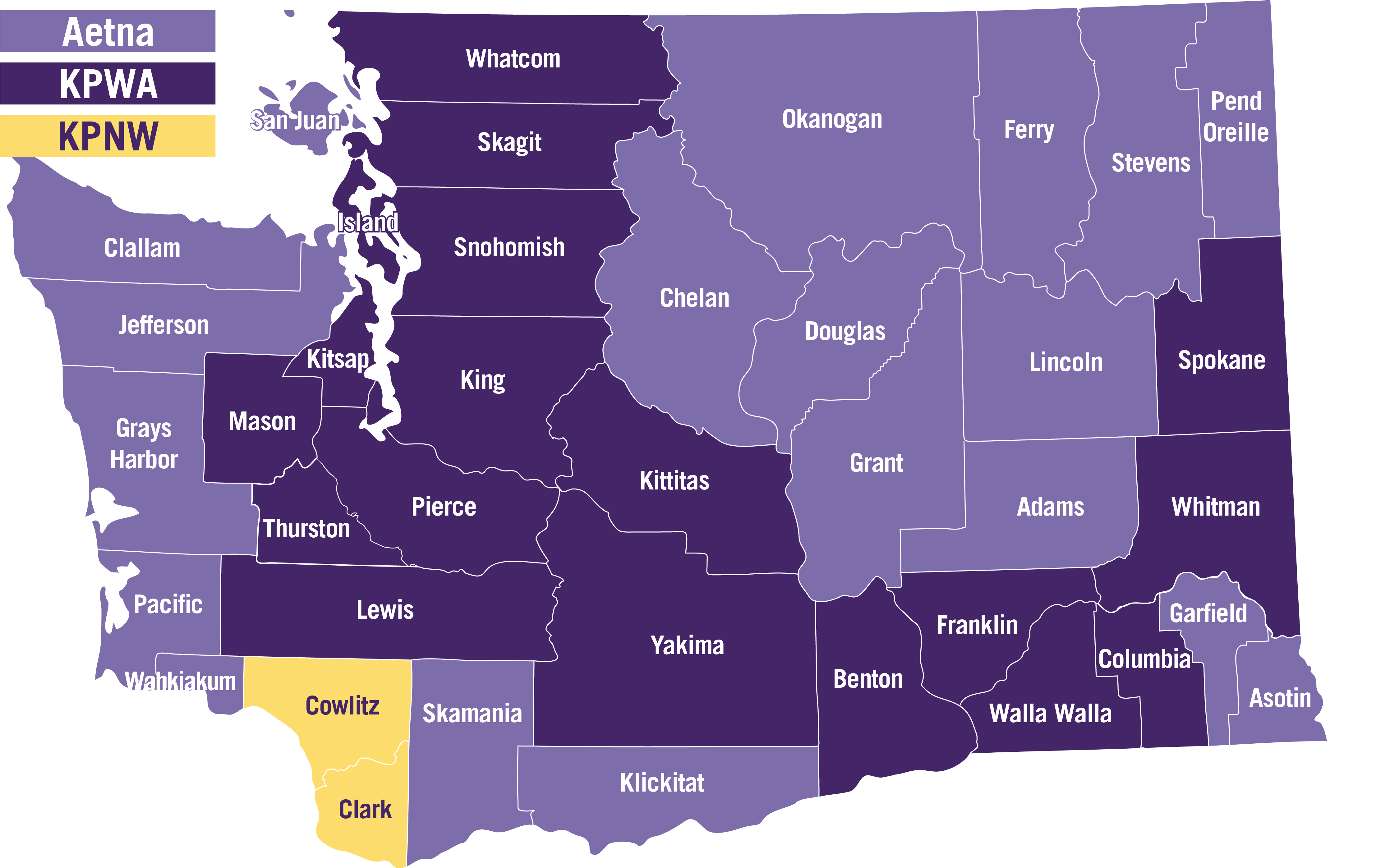 If you don’t know what plan you are on and need to find out, log into Health: My Plan or call SEIU 775 Benefits Group Customer Service at 1-877-606-6705.
If you don’t know what plan you are on and need to find out, log into Health: My Plan or call SEIU 775 Benefits Group Customer Service at 1-877-606-6705.
What is Dependent Verification?
When you enroll your dependent children, you will need to verify your relationship with them before coverage can begin. To do so, you must send a document for each child that you enroll. It is recommended that you submit your Dependent Verification document(s) with your completed Health Benefits Application. If you are unable to do so, you must submit your Dependent Verification documents(s) by September 30, 2023. If you send your Dependent Verification separately, please make sure to label it with your first and last name and the last four digits of your Social Security number. Learn more about acceptable dependent verification documents.
Which medical plan am I on?
Your medical plan is assigned based on your zip code.
If you live in the Kaiser Permanente Service Area (within 30 miles of a Kaiser Permanente of Washington (KPWA) or a Kaiser Foundation of the Northwest (KPNW) network provider), you are enrolled in either the KPWA or KPNW plan, depending on your ZIP code. If you are outside the Kaiser Permanente Service Area (KPWA and KPNW), you are enrolled in the Aetna plan.
NOTE: If you change your address, your medical plan may change. If your plan needs to change based on your new address, you will be notified in writing of the plan change.
Can my children and I have different medical or dental plan elections?
If you enroll your dependent children into coverage, they will be enrolled in the same plan that you are on.
Can my child be enrolled under both myself and my spouse?
Your child can only be enrolled in healthcare benefits through SEIU 775 Benefits Group (officially known as SEIU Healthcare NW Health Benefits Trust) one time; if you and your partner are both covered as caregivers, your child can only be enrolled by one parent. However, if your partner has healthcare coverage from another employer, both parents can enroll the child, which will then be covered by 2 healthcare coverage options.
What if my hours are reported to my employer late?
Hours worked must be reported to your employer within 60 days of the date worked to be used in the calculation of benefit eligibility. Your employer will report your hours worked to SEIU 775 Benefits Group. If your hours are reported late, hours will be recorded but coverage will not be extended.
Example: hours worked in January must be reported to your employer by March 31, and received by SEIU 775 Benefits Group from your employer no later than April 20 to ensure March coverage.
What happens if my monthly co-premium is not deducted from my paycheck?
If your co-premium is not able to be deducted from your paycheck, you will receive a self-pay notice to make the payment by PayPal using Health: My Plan, or by check or money order. If payment for your dependent coverage is not made, coverage will be dropped.
Mail your check or money order along with the self-pay tear-off to:
SEIU 775 Benefits Group
PO BOX 5349
Carol Stream, IL 60197-5349
What if I want to decline or end coverage?
If you do not want to enroll in healthcare coverage or would like to end your coverage and/or your dependent’s coverage (if you and/or your dependent are already enrolled), you can fill out the Waive Coverage form. If you choose to waive coverage, you will not be able to enroll again until the next Open Enrollment period (every year July 1-20) or if you have a Qualifying Life Event (QLEs).
If you submit a waiver on or before the 15th of the month, your and/or your dependent’s coverage will end on the 1st of the next month. If you submit a waiver between the 16th and 31st of the month, your and/or your dependent’s coverage will end on the 1st of the second month.
Example:
- If you submit a waiver between January 1 and January 15, your coverage will end on February 1.
- If you submit a waiver between January 16 and January 31, your coverage will end on March 1.
Health Plan Transparency
Starting July 1, 2022, your health insurance carrier is required by the Transparency in Coverage Rule to provide cost information about covered health services. Health plan price transparency will help you understand the cost of a covered item or service before getting care. Learn more about Health Plan Transparency.

